The minimally invasive tubular decompression is a workhorse procedure for spine surgeons. Patients complaining of leg symptoms with a focal disc herniation who have failed conservative options can undergo this procedure with great success. Most patients go home the same day, just a few hours after surgery.
- Good results are achieved in 80-90% of patients
- People with leg pain benefit more from surgery than those with back pain
- People with moderate to severe pain undergoing surgery tend to notice a greater improvement than those who did not undergo surgery
- Minimally invasive decompression has been shown to be as good or better than those undergoing open decompression.
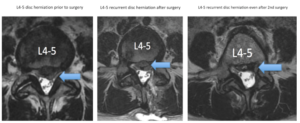
However, about 0.5-25% of patients will have a recurrent disc herniation at the same disc level.
There are many theories as to why someone develops a recurrent herniation. Obesity, smoking, diabetes, weightlifting and even the type of primary operation may be causative factors.
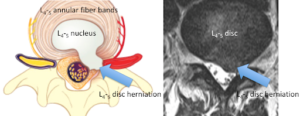
It is logical that one way for the surgeon to decrease the chance of recurrent herniation, would be to close the hole in the disc from which the herniation came. It is the center portion of the disc, called the nucleus (jelly-like material), which herniates through the outer disc bands, called the annulus fibrosis. After removing the herniated nucleus, the hole in the annulus remains. Surgeons have tried to find ways to close this hole and prevent more nucleus from herniating out, but it seems as though patients just need to wait for the hole to “scar over”.
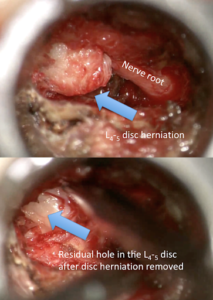 A new device, called the Barricaid- by Intrinsic Therapeutics- was FDA approved in February 2019. It is a titanium and polyester implant that can be placed over the hole in the disc’s annulus after the disc herniation is removed.
A new device, called the Barricaid- by Intrinsic Therapeutics- was FDA approved in February 2019. It is a titanium and polyester implant that can be placed over the hole in the disc’s annulus after the disc herniation is removed.
A recent study of 554 patients used this device and reported a 50% reduction in symptomatic recurrent disc herniation.
Further studies will be needed to confirm these results, but it may be a promising way to reduce recurrent disc herniations.
References
Atlas SJ, et al. Long-term outcomes of surgical and nonsurgical management of sciatica secondary to a lumbar disc herniation: 10-year results from the Maine Lumbar Spine Study. Spine, 30(8): 927–935, 2005.
Berjano P et al. Microdiscectomy for recurrent L5-S1 disc herniation. Eur Spine J. 2013 Dec; 22(12):2915-7.